9 Must-Know Facts About Colorectal Cancer
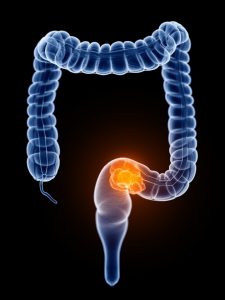
Colorectal cancer (cancer of the colon and rectum) continues to affect millions of men and women worldwide, and understanding the disease and what we can do to prevent it is the first step toward a cure.
Colorectal Cancer Statistics
- Colorectal cancer is the third most common cancer diagnosed in both men and women in the U.S.
- Although the death rate from colorectal cancer has been dropping for the past 30 years, it is still the second leading cause of cancer death in the U.S.
- The overall lifetime risk of developing colorectal cancer is: 1 in 21 for men and 1 in 23 for women.[i]
- There are currently more than one million colorectal cancer survivors in the U.S.[ii]
Here’s a list of nine facts you need to know about colorectal cancer. And make sure you read about related work by NFCR-funded scientists Dr. Wei Zhang, Dr. Daniel Von Hoff, Dr. Laurence Hurley and Dr. Yung-Chi Cheng.
1. With regular screenings, colorectal cancer is preventable.

Studies show that regular screening could prevent 1/3 of colorectal cancer deaths in the U.S. The five-year survival rate is 90% if detected early.[iii]
2. Age is the #1 risk factor for colorectal cancer.
90% of colorectal cancer cases appear in men and women 50 years old or older, and the risk for developing this cancer increases with age. Yet, like most disease trends, this isn’t absolute – younger people can get colorectal cancer too.
3. There are warning signs, but not EARLY warning signs.
Like lung cancer and cervical cancer, colorectal cancer can be hard to detect in its earliest stage. Symptoms can include a change in bowel habits; blood in the stool; diarrhea, constipation or feeling that the bowel does not empty all the way; frequent gas pains, bloating, fullness or cramps; weight loss for no known reason; nausea, tiredness and vomiting.[iv] If you experience any of these symptoms, contact your doctor right away.
4. Lifestyle choices impact colorectal cancer risk.

Other risk factors include heavy alcohol use, lack of exercise and diets high in red and processed meats. Additionally, cooking meats at a very high temperature can create chemicals on your food that may increase your cancer risk.
5. Family history matters.
People with a first-degree relative (parent, sibling, offspring) who has colorectal cancer have two to three times risk of developing this disease.[viii] A personal or family history of polyps (adenomas) also puts you at higher risk – especially if the polyps are large or if there are many of them.
6. Health conditions can increase your risk.
Your risk of colorectal cancer increases if you have the following conditions: Type 2 diabetes; inflammatory bowel disease (IBD), including either ulcerative colitis or Crohn’s disease; and having an inherited syndrome like Familial adenomatous polyposis (FAP) or Lynch Syndrome.[ix]
7. Regular colorectal cancer screenings typically begin at age 50.
8. There are different screening options.
Screening tests can include: colonoscopy; sigmoidoscopy; barium enema; CT colonography or virtual colonoscopy; and at-home tests like the fecal occult blood test, fecal immune testing or stool gene testing.[x] Talk to your doctor to see what screenings are most appropriate for you given your family history, age and lifestyle choices. For more information on cancer screenings, please refer to our.
9. Research helps us attack colorectal cancer – and all types of cancer.
NFCR has distinguished itself from other organizations by emphasizing long-term, transformative research that has the potential to save lives. Our scientists are conducting a wide range of cutting-edge research focused on improving diagnosis and treatment of colorectal cancer – and all types of cancer.
Studying the system of genes that form colorectal cancer

NFCR Fellow Dr. Wei Zhang
NFCR-funded scientist, Dr. Wei Zhang, is the Director of the Wake Forest Baptist Comprehensive Cancer Center’s Precision Oncology Initiative. Dr. Zhang has vast experience identifying biomarkers and genes in colorectal cancer. His current research team is studying how gene expression, gene amplification and mutations relate to and regulate each other. Using data from next-generation sequencing, Dr. Zhang’s team is identifying the genetic drivers or growth-promoting genes of a patient’s cancer.
Dr. Zhang has previously identified microRNAs (miRNAs) as biomarkers to improve colorectal cancer prognosis and predict treatment response. He used blood samples from healthy donors and patients with stage I through IV colorectal cancer, and confirmed that one microRNA molecule – miR-141 – may predict the outcome for stage IV colorectal cancer patients.
Chinese herbal medicine curbs colorectal cancer treatment side effects
Yung-Chi Cheng, Ph.D.
For approximately 20 years, with NFCR support, Dr. Yung-Chi Cheng, of Yale University’s School of Medicine, has explored the therapeutic properties of PHY906, a Chinese herbal medicine formula. Dr. Cheng and his laboratory team have discovered that cancer treatment with PHY906, combined with chemotherapy, alleviates the unpleasant gastrointestinal side effects of chemotherapy for colon and rectal cancer patients. Moreover, their research demonstrated that PHY906 also has its own, solo anti-tumor attributes. If there is continued success in clinical trials, PHY906 could become one of the first FDA-approved oral herbal medicines for anti-cancer treatment.
Targeted drug treatment and key colorectal cancer gene
The c-Myc gene is a cancer-causing gene (or oncogene) that is amplified in colorectal cancer and is a tough molecule in terms of finding targets for drug development. NFCR-sponsored scientists Dr. Daniel Von Hoff and Dr. Laurence Hurley are creating drugs to block large clusters of DNA called “super enhancers,” which control the expression of a network of genes – including the critical and seemingly-undruggable c-Myc gene.
Shutting down colorectal cancer through the blood stream

Dr. Harold F. Dvorak
Dr. Harold Dvorak received funding from NFCR for over 30 year and is responsible for the discovery of the vascular endothelial growth factor (VEGF). His discovery fostered the entire field of vascular biology and led to the development of VEGF-targeting anti-angiogenic drugs. Unlike other anti-cancer drugs that aim to directly kill tumor cells, drugs that target VEGF cut off the blood supply that tumors need to survive.
In 2004, the VEGF-targeting drug Avastin® was approved by the FDA for the treatment of colorectal cancer. More than 280 clinical trials are currently investigating the use of Avastin® in over 50 tumor types.
[i] https://www.cancer.org/cancer/colon-rectal-cancer/about/key-statistics.html
[iii] https://labtestsonline.org/understanding/wellness/e-over50-1/e-over50-4/
[iv] https://www.cancer.gov/types/colorectal/patient/colon-treatment-pdq
https://www.cancer.gov/about-cancer/causes-prevention/risk/obesity/obesity-fact-sheet
[vi] https://www.aacrfoundation.org/Science/Pages/obesity-and-your-cancer-risk.aspx
[vii] http://www.news-medical.net/news/20170208/Smokers-more-likely-to-die-from-colon-cancer-than-non-smokers-study-shows.aspx
[ix] https://www.cancer.org/cancer/colon-rectal-cancer/causes-risks-prevention/risk-factors.html
[x] https://www.cancer.org/cancer/colon-rectal-cancer/early-detection/screening-tests-used.html













